Dysfunctions in Blood Vessel Cells Linked to Albuminuria in Sickle Cell Disease
Written by |
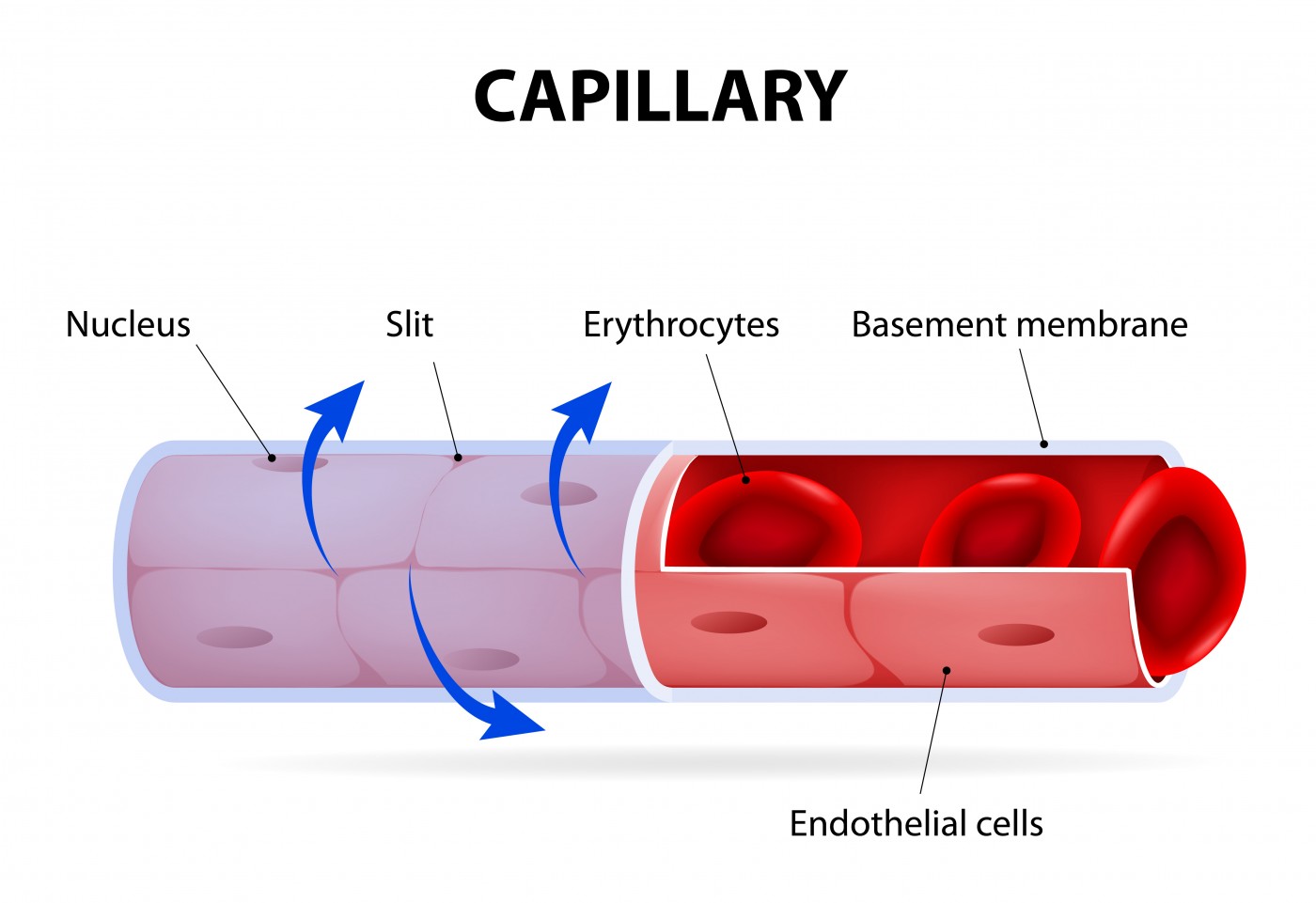
High levels of the protein albumin, a condition known as albuminuria and highly prevalent in sickle cell disease (SCD) patients, has now been linked to dysfunctions in cells that line the blood vessels (known as endothelial cells) in SCD patients.
The study, “Albuminuria Is Associated with Endothelial Dysfunction and Elevated Plasma Endothelin-1 in Sickle Cell Anemia,” was published in the open access journal PLOS One.
The development of albuminuria, (the presence of the protein albumin in the urine) in SCD is not completely understood. The prevalence of albuminuria increases with age, with estimates of between 4.5 and 26% of albuminuria in patients up to 21 years old, and between 26 and 68% in older patients.
Several studies have suggested that in SCD patients, albuminuria and increased levels of another protein, creatinine, are linked to vascular complications, including echocardiography-derived tricuspid regurgitant jet velocity (TRV), an important global marker for the severity and progression of SCD.
This suggests that dysfunction of components of blood vessels, such as endothelial cells (those lining the interior surface of blood vessels and lymphatic vessels) is a potential factor contributing to the development of albuminuria in SCD.
Here, a team of researchers studied how different parameters of endothelial function used noninvasive ultrasound imaging to assess the brachial artery, associated with albuminuria in patients with SCD. Urine samples from SCD patients were used to assess their albumin-creatinine ratio and 24-hour urine protein.
The scientists then correlated these results with patients’ endothelial function, determined by using brachial artery (the major blood vessel of the upper arm) ultrasound with measurements of flow-mediated dilation (FMD), nitroglycerin-mediated dilation (NTMD) and hyperemic velocity.
In total, the study enrolled 23 patients with SCD with a median age of 42 (range: 25-67 years old). Researchers found that the albumin-creatinine ratio is negatively correlated with FMD of the brachial artery, indicating its endothelium-dependent dilation. This represents the first physiologic parameter confirming the association of albuminuria with endothelial dysfunction in SCD.
Researchers also found that albumin-creatinine ratio correlated with several factors of endothelial function, including VEGF (vascular endothelial growth factor), plasma hemoglobin and ET-1 (endothelin-1); and with both 24-hour urine protein and urine aliquots for albumin-creatinine ratio obtained from the 24-hour urine collection.
These results support an association of albuminuria with endothelial dysfunction in SCD. Future studies are required to determine if medications that improve endothelial function can reduce the effect of albuminuria in SCD.