New Pre-transplant Treatment Regimen Improves Survival of Kids with Sickle Cell Disease, Trial Shows
Written by |
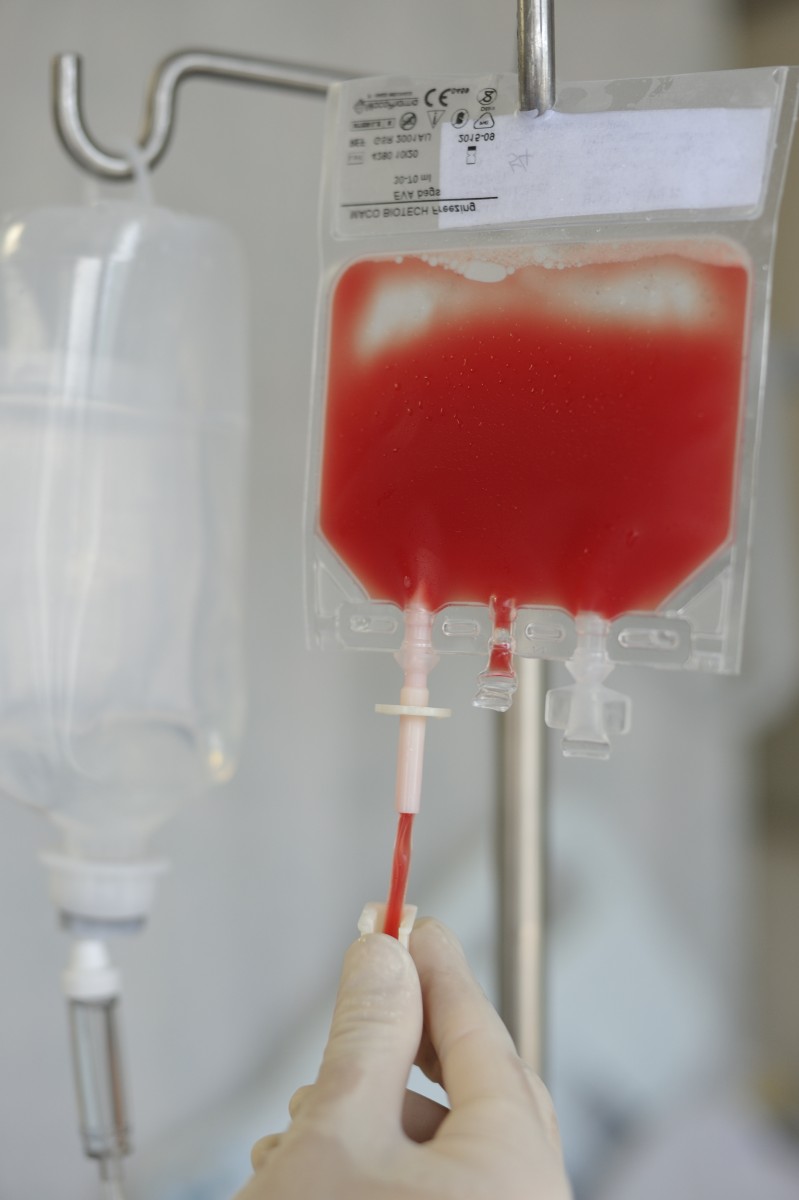
A new pre-transplant conditioning regimen remarkably improves rejection rates and survival in children with sickle cell disease (SCD), according to the results of Phase 1/2 trial (NCT00920972).
The study, “Unrelated Umbilical Cord Blood Transplantation for Sickle Cell Disease Following Reduced Intensity Conditioning: Results of a Phase I Trial,” appeared in the journal Biology of Blood and Marrow Transplantation.
Transplanting hematopoietic stem cells (cells that can develop into any type of blood cell) from matched sibling donors results in disease-free survival of greater than 90% in SCD patients. However, only about 18% of patients have suitable sibling donors.
Therefore, unrelated umbilical cord blood transplant (UCBT), which has been performed to treat diseases such as inherited metabolic disorders and primary immunodeficiency, became a viable alternative for patients with severe sickle cell disease and without a matched family donor.
But UCBT has been associated with high graft rejection rates of 50-62% and low disease-free survival (29-50%) in SCD patients.
A research team led by Shalini Shenoy, MD, hypothesized that the addition of anti-cancer and SCD agents hydroxyurea and thiotepa to a previously-tested reduced intensity conditioning (RIC) regimen — one that uses less chemotherapy and radiation to reduce health complications — would support engraftment (the growth and formation of healthy blood stem cells after transplant) in SCD patients.
Shenoy is a professor in the Division of Pediatric Hematology/Oncology at Washington University School of Medicine in St. Louis, Missouri.
Nine children ages 3 to 10 with complications from sickle cell disease underwent UCBT after conditioning with the new regimen. Immune system suppressants were used to prevent graft-versus-host disease (GVHD; transplant rejection).
Seven of the nine patients had successful engraftment and are free of sickle cell disease, and two recovered after a follow-up of approximately two years. Acute, mild, and moderate chronic GVHD developed in three, two, and one patient, respectively.
Four of five patients discontinued immunosuppressive drugs (medication to avoid rejection) two years after UCBT. In addition, seven patients recovered from viral infections. The one-year overall survival rate was 100%, and disease-free survival rate was 78%.
The study shows that UCBT is able to cure children with severe SCD, greatly reducing the incidence and severity of chronic GVHD. Importantly, the new “RIC regimen was successful in achieving sustained donor engraftment in the majority of SCD patients after UCBT in this phase I trial,” according to the trial results.
Because the study was conducted in a small group in a Phase 1/2 trial, confirmation trials in larger groups of patients are necessary. And, improving early infection and acute GVHD rates could make outcomes even better.
“Exploring conditioning regimens should continue so that this modality may benefit more patients with severe disease, until alternate curative options such as gene therapy are widely available,” the authors concluded.


